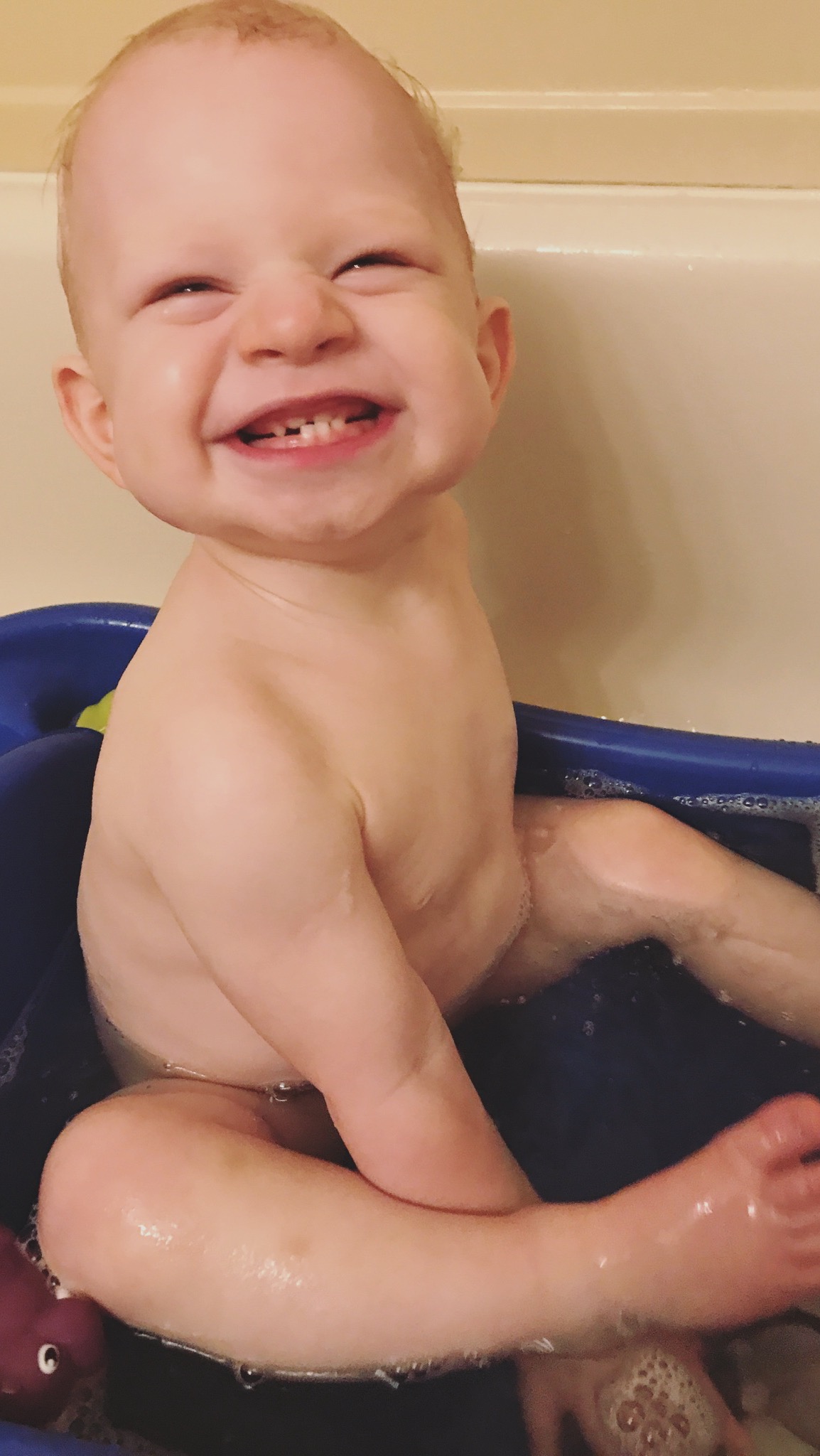
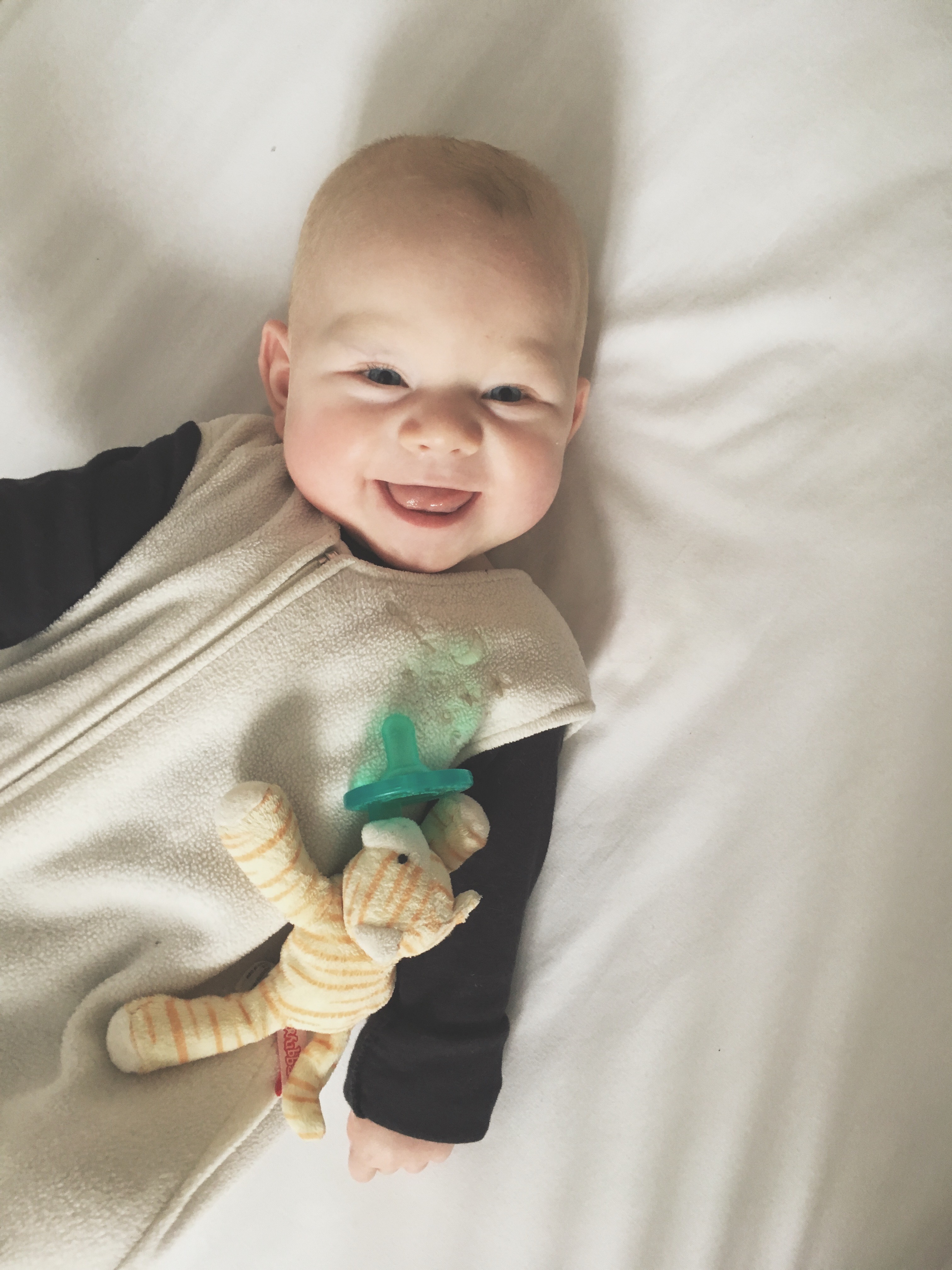
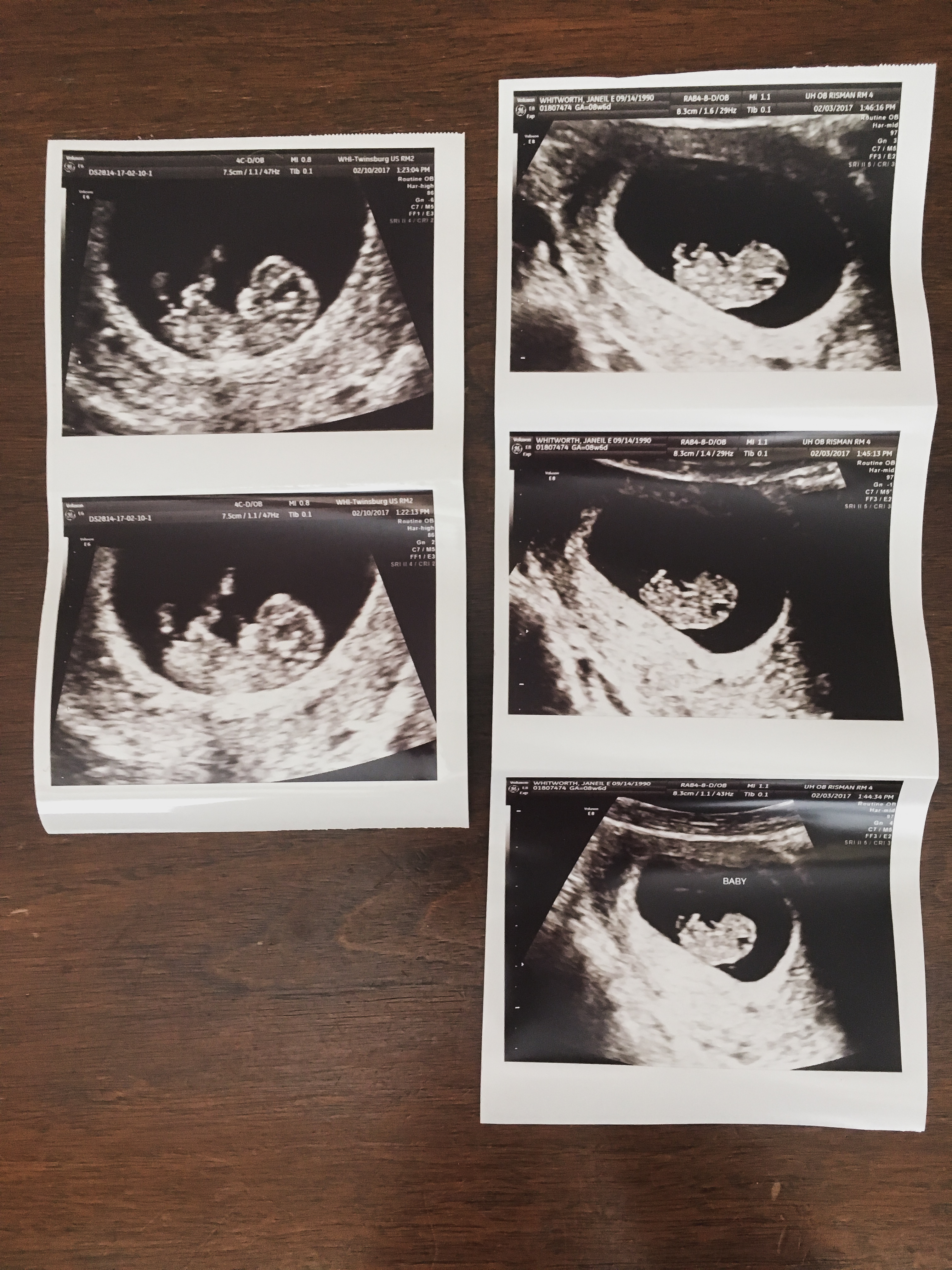
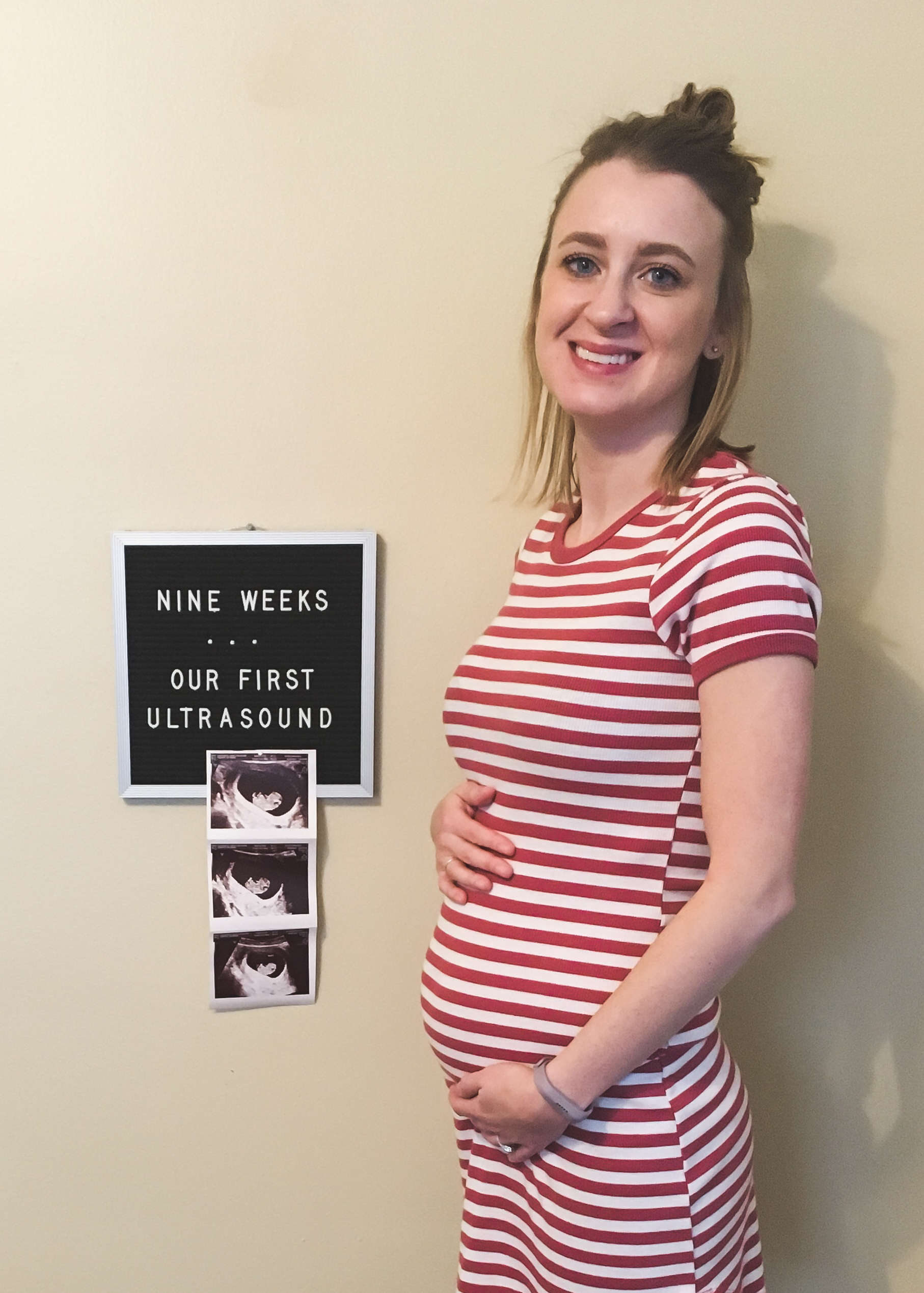
I absolutely love a birth story. They are narrations of incredible power and strength, vulnerability, immense joy, uncharted challenges, and unfortunately, sometimes deep grief—but always, always tales filled with bold love. Listen to a mother’s birth story and without fail, the ambient tone is love for her precious baby. I think it’s important to document a birth story because birth is a transformative event as it brings not only a baby into this world, but a mother. It’s the beautiful start of something dynamically everlasting: matrescence, or the act of becoming a mom.
—Here is Selby’s birth story.
Around 33 weeks pregnant, we noticed Selby’s growth was slowing down and my daily insulin requirements plummeted which was a red flag signally that my placenta wasn’t functioning properly. Early placental dysfunction is a rarer complication of diabetes in pregnancy, but it happens. To be safe, I was booked in for a 37 week induction to bring Selby earth side so he could continue growing outside the womb as soon as possible.
My pregnancy up until this point was not an easy one filled with many, many bumps in the road. In fact, the phrase “if she makes it that far….” was frequently thrown around at my appointments due to an early placental bleed, bout of preterm labor, IV antibiotics, high blood pressure, cystic fibrosis, CF related-diabetes, and never ending early contractions.
I wasn’t overjoyed at the idea of an early Pitocin induced labor but was ready to have our baby safely here. In the unmedicated labor and delivery world, Pitocin, the synthetic drug used to jump start labor, has a very bad rap. It can make contractions even more painful and intense than they would be naturally. I was totally aware of this fact going into my induction, but I tried to keep an open mind about what was to come.
The goal in birth is always just to have a healthy baby at the end of it, no matter how you end up getting there. However, because I experienced a precipitous labor with Fenn (labor lasting less than 4 hours from the start of contractions) my hope was for a more peaceful and slow ease into labor this time around. In contrast, I wanted the mental clarity and time to make decisions that I wasn’t granted with Fenn’s birth—such as bouncing on a birth ball if I wanted, walking around, pushing in different positions, reaching down to touch his head, experience the motions of labor, etc. I didn’t have the time or the mental space with Fenn to choose because his entrance was similar to a Midwest tornado—quick, forceful, consuming, jaw-dropping, unexpected.
Thankfully, my induction with Selby started in just that manner. At the beginning, it was almost boring with your typical Pitocin ramp-up starting after lunch, bouncing of birth balls, popsicles, and hospital TV. I made slow progress jumping from 2cm to 2.5cm at the start. At 5pm, I let the doctors break my water. I asked the doctors to wait to break my water delaying it for a hour, so I could get “there” mentally and eat another popsicle. I knew once they broke my water, my peaceful labor would end and be swallowed by a tidal wave.
“We are getting somewhere,” I said about two hours later through ragged moans. My contractions were close together and growing more and more powerful. With a popsicle in my hand bouncing on the ball, I asked the nurse where she thought I was.
“Four or five centimeters, maybe? Hard to telI.”
She asked if I wanted an epidural and I said maybe, but I wasn’t sure. I wanted to know how much longer before deciding. Our plan was to get back in bed and have them come check me and talk about the epidural thereafter.
Honestly, I should have known better.
I. Should. Have. Known. Better.
Two contractions went by as I stood up from the birth ball and desperately hung on to the IV pole breathing through the peak and fall. They were so incredibly powerful and concentrated that doubt started to fill my mind. I wasn’t going to do this naturally if it continued like that, I just couldn’t. I was at the edge.
They say history repeats itself.
And as if it was four years prior, a sudden all consuming urge to push came barreling through my body.
“Get them in here!!! Get them in here. I have to push, mom!”
I should have known better.
Peter ran and got the team in the hallway and I scrambled into bed with the help of my mom. I was briefly checked and declared to be 10cm dilated.
The nurses started the clock. Three minutes later, a few contractions, a touch of his head, some screams from me and then some screams from baby, a declaration of “It’s a BOY!”, and Sweet Selby was here.
A perfect 5lb 12oz baby boy born at 7:40pm out of a mix of God and science in multiple ways— fertility treatments, a miscarriage, an extremely high risk pregnancy, and most importantly highly effective treatments like Trikafta giving me this second chance at motherhood.
The flood of emotions knowing he was here was overwhelming. I couldn’t believe that I became a mom again after believing I wouldn’t be. History does repeat itself and it was glorious. Our nurses and doctors joyfully congratulated us with trembling voices matching mine. They excitedly chatted about how they didn’t expect his quick entrance and that I was born to birth. All women are born to birth—but it was an incredible compliment to the start of my matrescence with two.
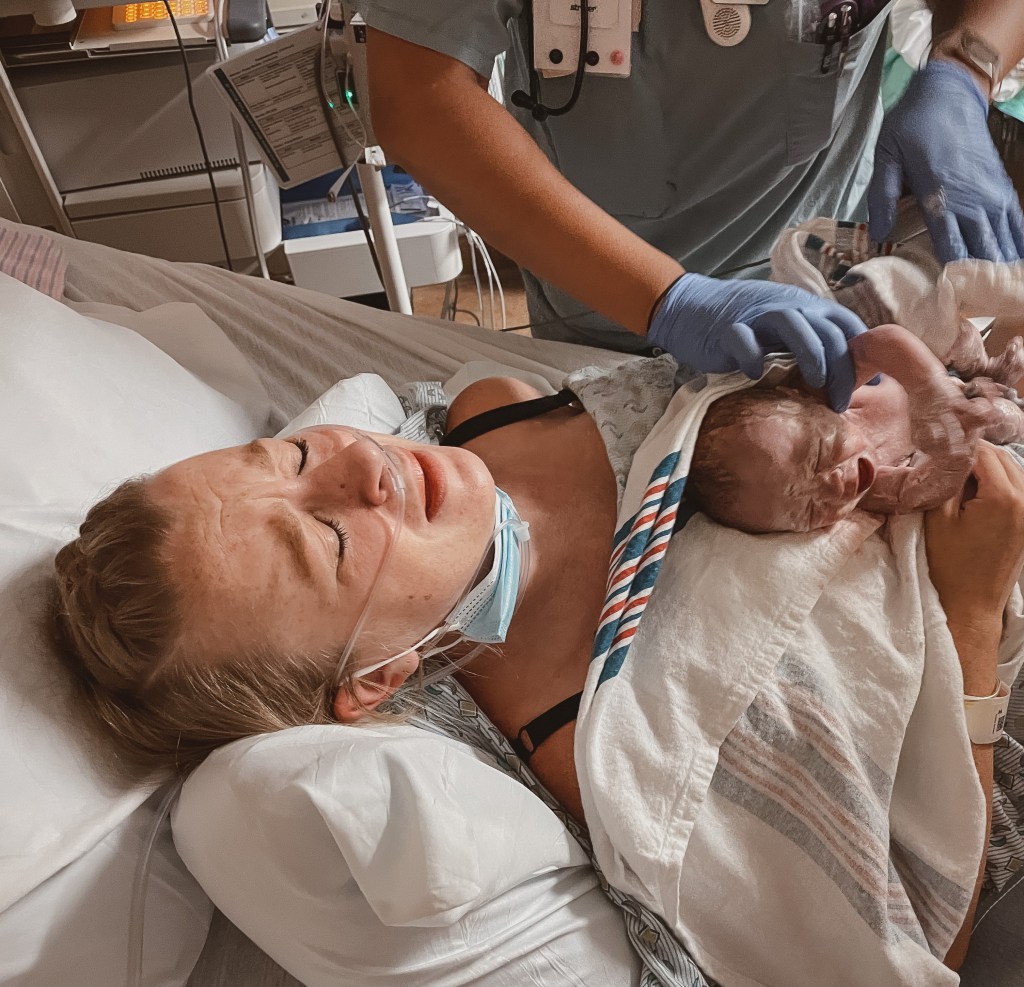
As Selby laid on my chest and we began to memorize his little face, the tone in the room changed. I was bleeding heavily and the medical team said I had clotting from a retained placenta. They massaged my abdomen uncomfortably to get contractions started but the bleeding continued. Next, I was given medications through my IV and had my bladder catheterized to relieve some of the pressure to allow my uterus to contract once more.
(Ugh, I went 31 years without having to ever be catheterized. That streak was now over. Selby gave me my first catheterization.)
When the bleeding continued, they stuck a different medication up my bum and called the attending on the floor to come do an ultrasound to locate the clots. I could see worried faces becoming more worried, but I was too focused on the little face beaming up from my chest.
Following, were some of the most painful moments I have ever experienced in my very long medical history. At this point I was still completely without pain medication after just having a rapid and forceful delivery. I felt every touch, pinch, and pull. The doctor explained she had to try to manually extract the clots from my uterus internally with her hand. Although necessary, they tried over and over again, and I wailed and tears fell down my face each time.
“I know this so terrible. I am so so, sorry I have to do this to you. Can you do one more time?” the doctor asked elbow deep.
I could do one more time, but each attempt was unsuccessful and the comforting voices around me began fading from fear.
After a few more tries, I told them I couldn’t do it again and that they had to give me something for pain. They said absolutely and pushed meds through my IV. I am someone who cautiously knows I love pain meds. It’s hard not to love pain meds when you live with chronic pain. So as the world got fuzzy and warm, I sunk in and gave them the “hang loose” motion asking them to not let the baby fall to the floor as I exclaimed I felt better and that they are all wonderful people. (I’m also really affectionate and encouraging on pain meds.)
Once the pain meds fully kicked in, the doctor warned if the next extraction didn’t work, I would be taken back to the OR for a D&C. They tried once more manually and she was finally able to extract the clots. The bleeding slowed down as my uterus began contracting again.
I enjoyed all the lidocaine and rode my high from Dilaudid as we breathed a sigh of relief and attempted to stitch me up. It was over–our sweet baby was here.
Labor can be brutal. It’s a high stakes game in an effort to gain the highest reward. I know people wonder why women choose to have unmedicated labors when there’s other options. I get it—it’s not everyone’s cup of tea.
However for me, each of my labors have healed me in a way. They have brought me peace in a body that’s often my enemy because of CF. I plead with my body everyday to work in my favor, sometimes in vain.
Breathe.
Digest.
Absorb.
Function.
Keep me alive.
Please.
It’s exhausting to work this hard in order to do the things a body was simply created to do. All that frustration and disappointment ultimately lands somewhere and makes a home in your mind after all those years.
In my heart, I know my body has been purposefully and wonderfully made, but sometimes I need a reminder. Bringing my babies into the world in this way–fiercely and uninhibited– is that reminder for me. It washes away the doubt that I am not a capable mother. It washes away the flecks of fear that I’m simply not physically strong enough for this life. It proves I am dynamic and not defined by my disease that defines nearly all my organs. I can barely stay alive, but I can bring forth life like a badass. And for me, there’s healing in that power no matter how silly it might be.
Fenn and Selby’s births are truly a labor of love and a means of encouragement to me that I am–and always will be–enough as their mother.
They are my most beautiful moments.







 Janeil
Janeil